Lack of dental bone can complicate or make implant placement impossible. Here we present different options for the placement of a dental implant in patients without bone or with little dental bone.
A) Causes of dental bone loss
Under ideal conditions, implants are placed in the patient's dental bone, which will serve as support for the installation of this anchor and the subsequent crown. However, some patients do not have dental bone or have an insufficient amount for the correct placement of an implant. Dental bone loss is a frequent problem, especially in advanced ages. Among the causes of this deterioration we find:
A1) Genetic causes
The loss or incorrect development of dental bone can be transferred from one generation to another due to various genetic diseases, such as cleidocranial dysostosis, cleft palate or Paget's disease. For this reason, it is recommended that parents who suffer from some type of genetic abnormality undergo genetic counseling before having offspring to assess the risk of their children inheriting it.

A2) Trauma
A strong blow to the maxilla or mandible can lead to wear or loss of dental bone. A review is recommended to see if the bone and the teeth themselves have been damaged in the event of having suffered an impact of this type. We recommend to all those who practice contact sports the use of protective splints on the teeth to avoid this type of risk.

A3) Diseases that cause wear or loss of dental bone
There are several ailments that can cause dental bone wear. Periodontal disease is one of the main causes of loss of bone structure, although not the only one. Oral tumors or certain types of infections such as pericoronitis or dental abscesses can also trigger this deterioration. It is important to carry out an exhaustive follow-up of these types of conditions in order to treat them promptly and minimize their consequences.
A4) Misaligned teeth
Having a misaligned denture or a malocclusion can trigger bad chewing that causes bone loss or prevents its proper development. To avoid these consequences, it is advisable to carry out a correct craniofacial study to assess possible solutions, which may include undergoing orthodontic treatment.

A5) Dental bone resorption
The absence of one or several teeth for a long time can cause the disappearance of the dental bone due to the lack of stimulation. For this reason, it is recommended to replace fallen teeth as soon as possible (within a year), even if it is a provisional solution while a final one is being prepared.

B) How to place implants in patients with little or no dental bone
It is time to present different alternatives for implant placement in this type of patient once the causes of bone loss have been exposed. We can distinguish between the use of implants adapted for these cases or the performance of techniques that allow the regeneration of dental bone.
B1) Implants for patients with dental bone problems
Dental implants are artificial roots, usually made of titanium, that are anchored in the bone, integrating into it. The common implant usually has variable height and width measurements depending on the amount of bone available and the patient's anatomy. In cases of patients with little bone we can use short implants, zygomatic or the all on four technique.
B1.a) Short implants
These implants have a shorter length and are usually indicated in patients with little bone or where the presence of anatomical structures prevents the placement of a longer implant. Sometimes, these prevent the need to regenerate the area previously with grafts.

B1.b) Zygomatic implants
The placement of zygomatic implants is another alternative to be able to rehabilitate a mouth in which the available bone is insufficient and one does not want to resort to bone grafts. The treatment consists of the placement of one or two implants of a longer length than the conventional ones that are anchored in the zygomatic bone or cheekbone. These can be complemented with the placement of conventional implants if the available bone allows it. Once placed, they can be restored with a fixed prosthesis in the same way as if they were conventional.
B1.ba) How is treatment with zygomatic implants performed?
It starts from an exhaustive previous study of the maxilla with the latest generation 3D technology. We can get the most out of the patient's bone with maxillary CBCT and three-dimensional study. It is evident that a complementary study of the patient's aesthetics is also needed: photographic analysis and study of models. Once the diagnosis is made, the treatment plan is explained to the patient. Normally zygomatic implants are complemented with two or more conventional implants in the anterior area. The placement of four zygomatic implants can be considered in cases where there is very little bone also in the anterior sector.

B1.c) “All on four” technique for implant placement
This technique allows the placement of four implants in both the maxilla and mandible. If the patient has lost bone in the posterior areas of the molars and the placement of implants is not feasible due to the interference of anatomical structures, the placement of these four implants will be in the lower jaw in front of the exit of the dental nerve through the mental foramen, and in the maxilla in front of the maxillary sinuses. A fixed prosthesis anchored on these four implants will be manufactured. This option is normally indicated in middle-aged or elderly patients who have decreased masticatory strength.

B2) Regeneration or grafting of dental bone to favor the placement of implants
The other possibility of installing implants in people with little bone structure is the performance of techniques that favor the recovery of this support. Within this category we find:
B2.a) Implant placement by bone expansion
Bone expansion allows the placement of implants in areas where the bone is narrower than normal. The procedure consists of performing a partial horizontal division of the bone, making it possible to place implants in the space created. Subsequently, the empty spaces are filled with biomaterials or autologous bone and a membrane is placed that covers the area. After 4 – 6 months, the implants will have integrated and a new bone volume will have been created.

B2.b) Block bone graft
This surgical technique makes it possible to regenerate bone defects in the indicated cases.~For this, small perforations are made in the bone of the recipient area to favor the correct vascularization of the graft. Subsequently, the bone block will be obtained, either from the patient himself or from a non-autogenous origin. Next, the remaining spaces are filled with particulate biomaterial and the area is covered with a membrane. After 4-6 months the bone will have been remodeled and it will be possible to place the implant.

B2.c) Guided bone regeneration
This is another procedure to regenerate the bone volume necessary to allow correct placement of the implant. For this, small perforations are made in the bone of the area to be grafted that will allow a correct vascularization of the graft. The primary goal is to create a space where new bone can grow and mature, which may require screw placement. Once the graft material is installed, a membrane is placed over it, which will allow bone remodeling and prevent soft tissue from entering the graft, which can interfere with bone regeneration.

B2.d) Atraumatic or transcrestal sinus lift
This technique consists of filling part of the base of the maxillary sinus with a graft material in order to obtain the necessary volume for the placement of dental implants. To do this, first prepare the support for the dental implant in the bone, reaching with the drills up to the cortex that forms the base of the maxillary sinus. The cortex is fractured in a controlled way with a special instrument to access the sinus and lift the Schneiderian membrane a few millimeters. Next, the graft material is introduced through the previously prepared hole, slightly compacting it inside the maxillary sinus. Finally, an implant can be placed immediately in the area if the quality and quantity of bone allow it. If this is not possible, it will be deferred until the bone regenerates correctly, around 6-9 months.
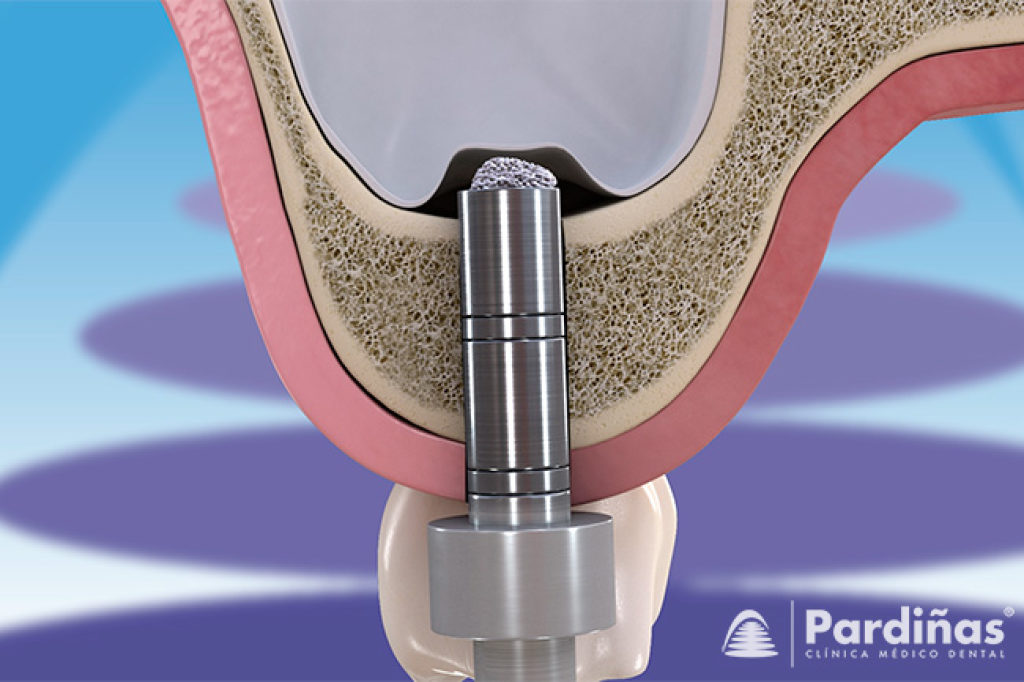
B2.e) Sinus lift with lateral window access
This also consists of filling part of the base of the maxillary sinus with a graft material that allows obtaining the necessary volume for the placement of dental implants. This technique is performed when it is necessary to obtain a greater volume and extension of bone. To do this, a "window" is opened in the lateral wall of the bone that forms the maxillary sinus. Subsequently, the interior of the maxillary sinus is accessed, carefully detaching the sinus membrane, and placing the graft material on the base of the sinus. The lateral window access is then sealed with a membrane and the area is sutured. If there is a minimum volume of bone that allows the placement of immediate implants, they can be placed; if not, its placement will have to be deferred until the graft has matured. The maturation time of the graft in the maxillary sinus is 6-9 months.

B2.f) Osteogenic distraction
This technique involves increasing the height of the alveolar ridge, favoring the formation of new bone. To do this, various devices are used that are anchored to the patient's bone and that, through successive activations, generate a fracture and controlled displacement of the bone fragments. Its use is not widespread and is limited to specific cases due to its technical complexity and the number of possible complications.